2015-01-22 05:00

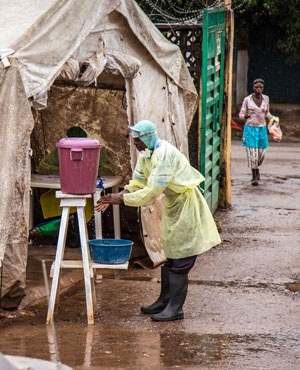
A health worker cleans his hands with chlorinated water before entering a Ebola screening tent, at the Kenema Government Hospital in Sierra Leone. (Michael Duff, AP)
Since it was launched about one month ago, the drive has doubled the number of ambulances for patients in the densely populated west of a country where more than 3 000 people have died.
Police halt vehicles at checkpoints in the tumble-down streets to check temperatures, while posters proclaim in the local Krio language: “Togeda we go stop ebola.”
Aid workers also report success in changing behaviour in rural areas, notably discouraging people from burial rituals involving direct contact with the dead – a major source of transmission.
As a result, transmission of the haemorrhagic fever has slowed sharply in the West African country, which has recorded more than 10 000 cases since May. There were just 184 new cases in the week to 11 January – the lowest in five months.
More than half of beds in treatment centres across Sierra Leone are now empty – a stark contrast from a peak in November when centres in Freetown overflowed, patients waited days for ambulances and bodies were unburied, or interred secretly in backyards.
This has prompted President Ernest Bai Koroma to say he believes his government – helped by the nearly 800 British soldiers and more than $450m in foreign aid – can stamp out Sierra Leone’s last case by the end of March.
Some health specialists and aid workers are more cautious.
They hope the success in Freetown and its environs is a big step towards beating the epidemic – which has killed more than 8 400 people – now that Liberia and Guinea also appear to have stabilised, but are wary of calling the end of an outbreak that last April seemed to wane in Guinea, only to return ferociously.
Operation Western Area Surge
“The Sierra Leone problem is turning the corner. I think we’ll get close to zero there by March so long as there are no surprises,” said Philippe Maughan, senior Ebola operations manager at ECHO, the European Commission’s humanitarian aid branch.
“But … there will be cases popping up here and there over the next six months to a year and we’ll need to snuff them out.”
United Nations Ebola chief David Nabarro told the World Economic Forum in Davos on Wednesday that UN agencies needed a final $1bn to fight the epidemic in West Africa.
The National Ebola Response Centre (NERC), a new military-style body chaired by Koroma, launched “Operation Western Area Surge” last month in Sierra Leone – a country of six million people where the main industries are fishing and farming but which has huge, largely untapped, mineral reserves.
A jingle is played repeatedly over loud speakers at the command centre: “Ebola go, we don’t tire!”
Freetown’s main Kingtom cemetery has been expanded and highly contagious bodies are buried in deep graves within 24 hours according to strict protocols to prevent transmission.
Burials are important in West African culture, with mourners often touching the corpse in intimate, spiritual farewells to their loved ones. Ebola spreads via contact with bodily fluids of infected people or with corpses of someone killed by it.
The Ebola centre has noted pockets of resistance in the capital, which officials attribute to mistrust of authorities due to the weak response before the surge.
In one home in the Devil Hole neighbourhood outside Freetown where a nine-year-old boy was taken away by medics, relatives said he caught Ebola from malaria drugs handed out by the government.
“The challenge is this last small group of people who aren’t changing their behaviour,” said Joanna Reid, head of Britain’s Department for International Development in Sierra Leone. “That’s the last mile.”
Changing behaviour
Aid workers say overcoming misperceptions and changing behaviour was critical to breaking transmission chains in rural hotspots like Kailahun, where case counts have fallen to zero. The same must now happen in Freetown, they say.
David Heymann, head of Britain’s Chatham House Centre on Global Health Security, said both current success and future progress is largely due to communication.
“They’ve finally got strong communication … probably through traditional leaders and others who are helping communities understand how to prevent transmission. From my past experience with outbreaks, when communities learn how to communicate the risks and how to prevent infection, the outbreak stops – it’s as simple as that.”
Some are taking matters into their own hands, such as Ebola survivor Mohamed Mansaray, 61, who lost six family members to the virus in the fishing village of John Thorpe on the outskirts of Freetown.
“People were attributing the deaths to witchcraft, that’s why people died,” Mansaray said, sitting on a bench beneath a mango tree. Calling himself an “Ebola Evangelist”, he goes from house to house trying to educate locals about the disease.
In a sign of change, John Thorpe residents are starting to hand over the sick to a new centre built by charity Oxfam.
It has proved harder to change attitudes in Freetown than in rural areas, despite a high case density there of one in around 300 people – a factor that would normally increase awareness.
A November survey showed less than half of respondents in and around Freetown had comprehensive knowledge of Ebola – the nation’s lowest level.
“In Freetown, many live roaming lives so the possibility of transmitting correct messages is lower than in rural districts,” said British anthropologist Paul Richards, who has 30 years of experience in Sierra Leone.
He said some people resisted because stopping transmission involved attacking key cultural values: “You have to abandon some of the basic features of being a good person – visiting the sick and doing the decent thing for the dead.”
Nine contacts
In a positive sign, the percentage of corpses picked up by burial teams around Freetown testing positive for Ebola has dropped below ten percent, from 30% before the surge, as families report suspected cases for treatment earlier.
There is still much to be done. There is not yet a central database of Ebola contacts and there are only nine contacts for each Ebola case, versus an average of 10-15 for Liberia.
Even if contacts are established, officials often get lost searching a country with no postcodes and where street numbers are often not sequential.
Speaking from the NERC situation room, a converted court room used to try criminals from the 1991-2002 civil war, its director OB Sisay says a key challenge is deploying resources quickly.
NERC needs approval from partners like the World Bank to allocate budgets – a safeguard against embezzlement.
“Let’s say I need food to quarantine a community. It can take two weeks,” said Sisay in an interview interrupted every few minutes by demands from medics and local chiefs.
Since Guinea’s outbreak began in December 2013, officials have become aware Ebola can rear up from a single imported case, as occurred in Mali in October.
President Koroma now wants to decentralise the Ebola response to handle isolated rural cases. But in a densely-forested country where less than 10% of roads are paved, it’s hard to get patients in the “wet phase” – vomiting and sometimes bleeding from the eyes and ears – into care.
“We are getting there,” said Karline Kleijer, operations manager for Medicins Sans Frontieres in Sierra Leone. “Major steps have been made, but we still have a long way to go.”



